Women’s health screening in 2026: Why combining GP assessment, ultrasound and genetics delivers better outcomes
Article produced in association with Spital Clinic and Jeen Health
The Women’s Health Strategy for England, published in 2022, identified significant gaps in how women’s health needs are met across the life course.
Among the issues highlighted were poor access to specialists, delays in diagnosis for conditions such as endometriosis and PCOS, and a healthcare system that has historically addressed women’s health in episodic fragments rather than as a coherent whole.
Four years on, the private sector has responded in part by developing more integrated models of care, combining clinical consultation, specialist imaging and genetic risk assessment within a single service framework.
The Case Against Siloed Healthcare
Standard NHS provision for women’s health is built on discrete pathways: a GP for general health, a gynaecologist for reproductive concerns, a radiologist for imaging, and a genetics team for hereditary risk.
Each of these services operates with its own referral criteria, waiting times and communication systems.
The result for the patient is that related health concerns are addressed separately, often without the practitioners involved having access to each other’s findings.
This is not a failure of individual services but a structural feature of how healthcare is organised.
For complex conditions that span multiple clinical domains, such as a woman with a family history of ovarian cancer, irregular cycles and unexplained pelvic pain, the episodic model creates delays and requires the patient to navigate between services rather than being assessed as a whole person.
What Integrated Women’s Health Screening Covers
A comprehensive private women’s health screen in 2026 typically encompasses several components that are rarely offered together within the NHS framework:
- General health assessment: blood pressure, BMI, thyroid function, iron levels, cholesterol and diabetes risk
- Cervical health: smear test, HPV testing and, where indicated, referral for colposcopy
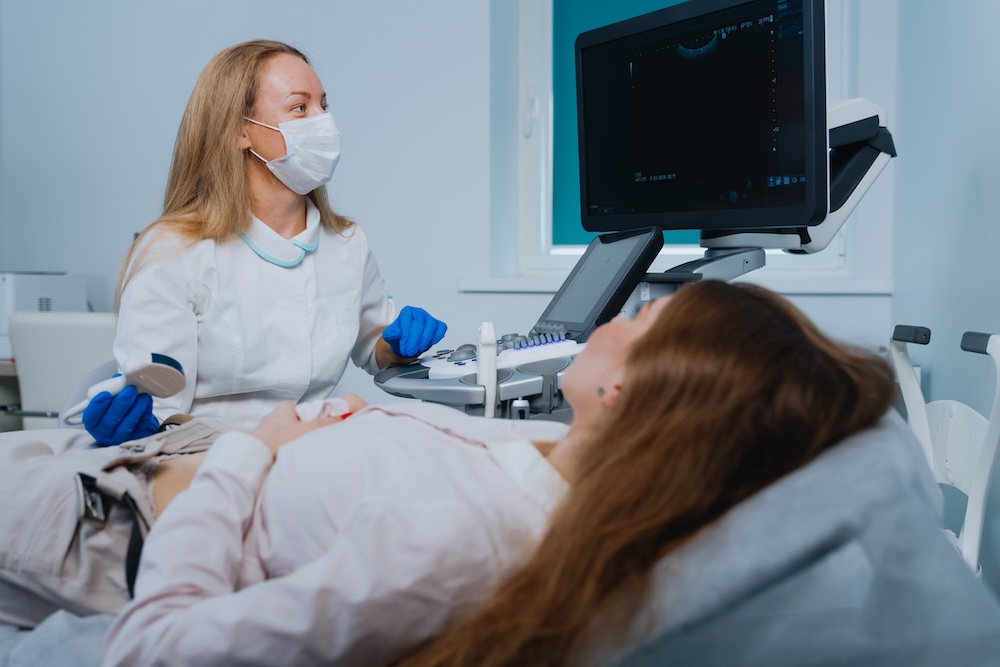
- Pelvic ultrasound: assessment of the uterus, ovaries and adnexa, identifying conditions such as fibroids, ovarian cysts and endometrial abnormalities
- Hormonal assessment: oestrogen, progesterone, FSH, LH and AMH where relevant to age and symptoms
- Genetic risk assessment: carrier screening, hereditary cancer risk testing and, where indicated, genetics counselling
Receiving all of these assessments together, with a single clinician or team coordinating findings, provides a more complete picture and reduces the risk of clinically significant findings being overlooked.
Spital Clinic’s Approach
Located at Spital Square in the City of London, Spital Clinic operates as a multidisciplinary private clinic offering general practice, gynaecology, ultrasound scanning, sexual health and specialist screening within a single clinical environment.
For women who want a comprehensive annual health check, or who present with specific concerns, this model reduces the administrative burden of managing multiple referrals and appointments across different providers.
The clinic offers appointments seven days a week including evenings, which is a practical consideration for women in full-time employment who are unable to access daytime NHS appointments.
The Role of Genetic Testing in Integrated Screening
Genetic risk assessment adds a dimension to women’s health screening that routine clinical and imaging assessments do not cover.
For women with a family history of breast, ovarian, uterine or colorectal cancers, or for those who have concerns about hereditary conditions, incorporating genetic testing into a regular health screen provides information that informs not just current management but long-term health planning. Jeen Health offers a range of genetic testing options, including hereditary cancer risk panels and carrier screening, which can be accessed independently or as part of a coordinated assessment alongside clinical services.
How the NHS Women’s Health Strategy Frames This
The Women’s Health Strategy sets out ambitions for improved access to care, better information, and services that treat women’s health comprehensively rather than condition by condition.
It also acknowledges that NHS capacity will not deliver all of these ambitions immediately.
Private providers who have built models of integrated care are, in effect, demonstrating what is achievable when organisational barriers are removed.
This is not to suggest that private care is a universal solution; access remains a significant equity issue.
But the clinical model that integrated screening represents is instructive for how NHS services might evolve. The evidence that early identification of risk factors leads to better outcomes is not in dispute.
A Note on Annual Screening
There is ongoing clinical debate about the value and appropriate scope of annual health screening in otherwise well individuals.
The principle is sound where tests are targeted at conditions with effective early interventions.
The key is that a comprehensive health check should be guided by individual clinical risk rather than being a one-size-fits-all approach. Specialist private providers are well positioned to tailor screening to individual circumstances rather than following a standardised menu.
Disclaimer: This article is produced for informational purposes only and does not constitute medical advice, diagnosis or treatment.
Clinical guidance referenced reflects published NHS, NICE and RCOG standards as at March 2026. Individual circumstances vary; readers are advised to consult a qualified healthcare professional before acting on any information in this article.
This piece was produced in association with Spital Clinic and Jeen Health, which provided background clinical information for editorial purposes.
Hyperlinks to external sources are included for reference only and do not represent an endorsement of any product, service or organisation.