New technology for the diagnosis and treatment of cystic fibrosis has been granted FDA approval for clinical use in the USA.
Scientists at Monash University have developed non-invasive technology which is able to pinpoint localised areas of deficiency in the lungs, allowing for earlier, faster and more accurate diagnoses.
They believe the research could hold the key to better monitoring and treatment of lung disease associated with cystic fibrosis.
Cystic fibrosis is a progressive, chronic and debilitating genetic disease that begins early in infancy and produces a steady deterioration in quality of life, ultimately leading to premature death.
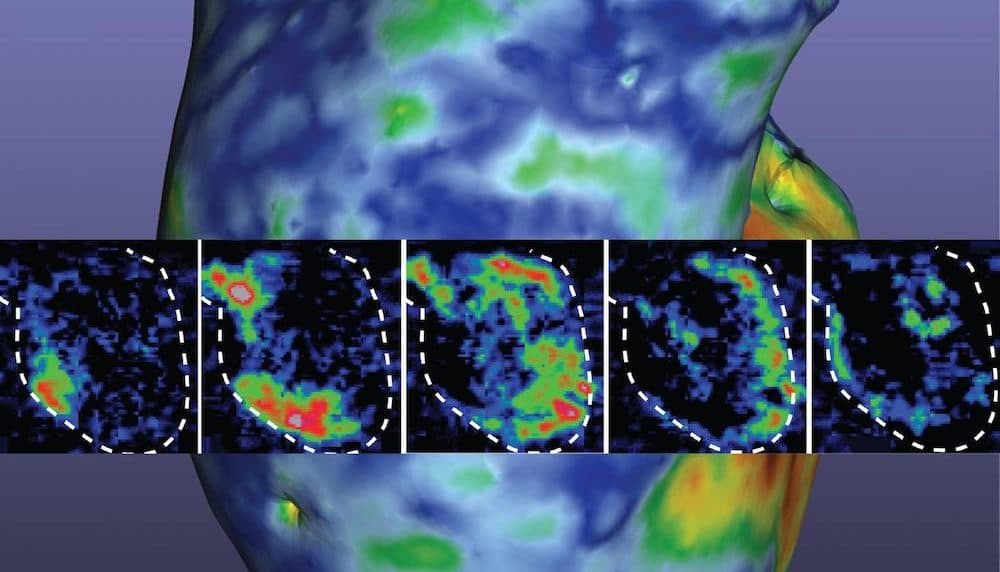
The technology, known as X-ray velocimetry (XV), can track the movement of air through the lungs, making it possible to identify the exact locations of abnormal airflow and quantify the level of disease present.
Dr Freda Werdiger, of Monash University’s Department of Mechanical and Aerospace Engineering, who led the study, says: “Although we know a lot about what kills cystic fibrosis patients, not a whole lot is known about the specific stages of cystic fibrosis. What my paper did is identify a new way to quantify the disease at its different stages.”
Currently the most common method for testing lung function is through spirometry, which involves patients breathing into a device which measures their lung capacity.
Later in the testing process, CT scans are used to detect more serious abnormalities, such as structural damage and mucus plugging.
Werdiger explains: “With spirometry, you use the results to look at people’s progress; whether they are better or worse than before. With this technology, we are able to make airflow data visual, describing presentations of the disease and then quantifying them.”
XV technology is able to combine structural and functional imaging in one test at a lower radiation dose than current technology. It also eliminates the need for contrast, a special dye injected into the body before a CT scan.
Werdiger says this new field of functional imaging and the non-invasive nature of the technology will improve the quality of life of children with cystic fibrosis.
She says: “Children that have cystic fibrosis spend so much of their lives going to get tested. XV gets a lot more done in a shorter period of time, so they don’t have to go in for testing so often.”
XV technology is also expected to have the potential to improve the detection and management of other lung diseases, including lung cancer.
“The problem with a lot of lung diseases is that by the time the damage is enough to see structural changes, it’s already gone quite far,” Werdiger says, “so by the time something is visible on a CT scan, the structural damage is already there.
“When you have deposits in the lung due to cancer, for example, you would never be able to pick that up with spirometry because it’s at the mouth, whereas we can see where there is a limited airflow and go on to do more investigation.”
XV technology was designed and commercialised by Australian-based med-tech company 4DMedical, led by CEO and former Monash University researcher Professor Andreas Fouras.
Whilst working on research using wind tunnels, Fouras identified properties that could be adapted to understanding airflow in the lungs.
After 15 years of animal and human testing, the technology has been upscaled for clinical use and was recently given FDA approval in the USA for all respiratory indications in adults.
Werdiger says, “When it comes to this functional imaging, now that we have the technical capabilities, it’s really important that any quantities that we pull from the images are intuitive for clinicians.”
4DMedical is a medical technology company specialising in respiratory diagnostics for all lung disorders including: coronavirus, asthma, COPD, cystic fibrosis and cancer.
See more at 4dmedical.com