
Joe Fernandes, founder and CEO of BuzzStreets, assesses the current vision in healthtech and what that means for future innovation
The future has a way of creeping up on us. Someone who grew up watching Star Trek (the original series) can now stream the adventures of Kirk and Spock on their phone. But the journey from ‘wouldn’t a communicator be cool’ to having a device that is objectively so much cooler is such a long one that few of us take time to marvel at this now ubiquitous and indispensable piece of technology. But that is how it is with the future – suddenly it is here. And we rarely notice its arrival.
However, the future does not just happen on its own; the present needs to have a vision of what the future might be. And within the health sector there is currently an impressive amount of vision.
 The top five answers to a Family Fortunes question about things associated with hospitals would likely lean towards Doctors, Nurses, Patients, Beds and Medicine, and that is unlikely to ever change. But what about the rest of the top ten. Ambulances? Bedpans? Masks? Needles? Wheelchairs? They are probable answers now, but in the future, the top ten may include 3D Printing, Artificial Intelligence, Nanomedicine, Robotics and Wayfinding.
The top five answers to a Family Fortunes question about things associated with hospitals would likely lean towards Doctors, Nurses, Patients, Beds and Medicine, and that is unlikely to ever change. But what about the rest of the top ten. Ambulances? Bedpans? Masks? Needles? Wheelchairs? They are probable answers now, but in the future, the top ten may include 3D Printing, Artificial Intelligence, Nanomedicine, Robotics and Wayfinding.
3D Printing
Additive manufacturing is where a digital file is used to create physical objects by adding multiple layers – it is more commonly called 3D printing. The origins of the concept are found in the early 1980s and since then more than a dozen methods or technologies have evolved, with examples of 3D printing in medicine (actual and potential) including organ and tissue manufacturing; personalised medical equipment; customised implants and prosthetics; anatomical models for education and surgical planning.
California-based Organovo is one of the leaders in the research and development of 3D bioprinting; they have a goal of 3D printing patches made of human tissue for defunct organs and entire organs for transplantation.
Artificial Intelligence
Healthcare use of artificial intelligence (AI) is expected to grow rapidly. Examples of ways that AI could reduce and/or mitigate risk include: helping to detect high risk patients by identifying those in need of medical intervention and triggering alerts to medical staff; and helping to deliver personalised recommended dosages by factoring in the unique body chemistry and associated environmental factors associated with individual patients.
[activecampaign form=11]The UK’s Babylon Health has a patient-centered remote consultation service that, through deep learning, can provide users with personalised insights to help them to better understand their health.
Nanomedicine
Nanomedicine applies the tools of nanotechnology to the treatment and prevention of illness. It involves the use of nanoscale materials for the delivery of therapeutics (including vaccines), biomarker discovery, bioimaging and for the treatment of neurodegenerative diseases.
There are a number of start-ups around the world with interesting projects, including Israel’s Vecoy Nanomedicines looking to treat viral infections by administering novel nano-scale virus-traps that capture and destroy viruses.
Robotics
Surgical Robots are machines that execute surgical tasks. But they are not autonomous. A (human) surgeon performs the surgery using robotic instruments that they guide via a console. Although tiny wristed instruments move like a human hand, they have a much greater range of motion. The small size of the instruments means surgeons can operate through one (or a few) small incisions, helping with complicated operations by allowing greater precision and flexibility than traditional techniques.
Globally, da Vinci surgical systems is the oldest and most widely used system in this field.
Wayfinding
Wayfinding is an important step forward in making hospitals become more patient-oriented. It also saves the hospital time and money.
More than 85 per cent of patients ask for directions when they go to a hospital or other public health facility, and 30 per cent of first-time visitors get lost (Source: Deloitte Digital). Wayfinding enables patients and other visitors to navigate from outside the hospital all the way to the specific location they need, whether that is a bed on a ward, a consulting room, the café, or the pharmacy.
This saves staff time; many times a day doctors and nurses are stopped (and therefore delayed) by visitors asking for directions; and often patients are late for appointments as they are lost within the hospital. Indoor Wayfinding solves both these problems.
Global positioning systems are part of everyday life and, in normal times at least, help to guide millions of people and vehicles down roads and pavements every day. Since the arrival of Google Maps, we are used to reliable digital navigation outdoors, so it’s an obvious next step to take this navigation indoors.
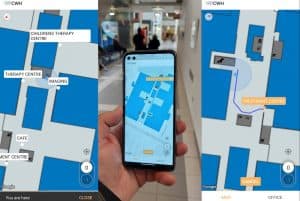 For example, BuzzStreets technology helps people navigate easier through a hospital as well as giving them a more independent experience. The navigation app can personalise the route, so if you want to avoid the stairs it will show you how, it can also choose the fastest or least busy route for you, plus it can highlight interesting features along the way, for example, it can tell you more about the art on the walls of the corridors.
For example, BuzzStreets technology helps people navigate easier through a hospital as well as giving them a more independent experience. The navigation app can personalise the route, so if you want to avoid the stairs it will show you how, it can also choose the fastest or least busy route for you, plus it can highlight interesting features along the way, for example, it can tell you more about the art on the walls of the corridors.
BuzzStreets also includes features such as a communication system between patient and doctor, the possibility of scheduling appointments, receiving medical scans and prescriptions in the app, heat maps, contextual notification, updated and edited locations, appointment reminders, and multilingual voice guidance. All of these features, and indoor Wayfinding in general, have a direct and positive contribution to the experience of patients, staff and visitors.
The BuzzStreets system can be found in a few pioneering hospitals, including the Chelsea and Westminster in London.
In conclusion, an agile approach to the development and adoption of new technology has allowed the NHS to reimagine what is possible, from healthcare consultations via video calls, to supporting X-ray diagnostics with machine learning algorithms. As well as valuing and supporting healthcare workers, tackling red tape and bureaucracy, embracing the private sector, and improving collaboration between NHS organisations and external providers.
Ultimately, the hospitals of the future are those that are focused on creating a better and more personalised patient experience.










